By Samkelo Mahlalela | 2019-09-12

The HIV and AIDS epidemic has been a concerning issue for the Kingdom of Eswatini, since the first case of HIV was reported in 1986.
The early years were particularly difficult as there was not much information known about the disease and there were no treatment options, leading health practitioners and academics to predict that the epidemic would wipe out the whole population, it was projected that the country would experience a negative population growth rate by 2004.
Today however, new HIV infections have reduced by 44 per cent since 2014 and by the year 2017, the initiation of people living with HIV (PLHIV) on antiretroviral therapy (ART) had been accelerated to reach 85 per cent of PLHIV, with 92 per cent of those virally suppressed.
The HIV prevalence has stabilised to 27.4 per cent, and to date, over 70 000 AIDS-related deaths have been averted since the introduction of ART in 2003. These key indicators suggest that the country is on the right trajectory to ending AIDS as a public health threat.
However, despite these achievements, there remains many concerning issues in the Eswatini HIV response and the global community. In the over three decades of responding to HIV, stigma and discrimination PLHIV and those populations at increased risk of HIV transmission still exists to varying degrees.
In June 2016, the United Nations General Assembly (UNGASS) having agreed that ending AIDS by 2030 requires a fast-track response set a target to reach three milestones by 2020.
Importantly, the third milestone is to, “eliminate HIV-related stigma and discrimination by 2020”.
The National Multisectoral HIV and AIDS National Strategic Framework (NSF) 2018-2023 recognises and incorporates the global strategy, as seen in its vision to super fast-track the HIV response to achieve: 85 per cent reduction of new HIV infections; avert 50 per cent of deaths among PLHIV; and Elimination of HIV stigma and discrimination.This means that eliminating stigma and discrimination is a priority in Eswatini’s HIV response.
Stigma and
discrimination
Stigma is the process of devaluation of people either living with HIV or associated with the illness.
Stigmatisation can take various forms, including being discredited, seen as a disgrace, and or perceived to have less value. When stigma is acted upon (also referred to as “enacted stigma”), the result is discrimination - the unjust treatment of individuals based on their real or perceived HIV status.
Discrimination consists of actions or omissions that are derived from stigma and directed towards those individuals who are stigmatised.
HIV-related stigma often builds upon and reinforces other existing prejudices, such as those related to gender, sexuality and race.
Typically, the stigma associated with HIV is often based upon the association of HIV and AIDS with already marginalised and stigmatised behaviors such as sex work and same-sex and transgender sexual practices.
HIV-related stigma affects those living with HIV and through association, those that they are associated with, such as their partner or spouse, children, and other members of their household.
Stigma, discrimination and human rights prohibitions are barriers that hinder access to HIV services.
Among PLHIV, self-stigma and fear partly accounts for late initiation on ART, especially among men, and hinders status disclosure and adherence to treatment.
As a result, most people testing HIV positive prefer to seek treatment services in distant health facilities where they are not known.
On the other hand, discrimination deters people from getting tested; it discourages open dialogue and safe practices (around issues of HIV and AIDS in general, condom use, and support for PLHIV), and lowers self-esteem, thus increases the spread of HIV and AIDS.
The Multiple Indicator Cluster Survey (MICS) 2014, showed a drop in the percentage of people who report accepting attitudes towards people living with HIV, from 47.1 per cent in 2010 to 37.4 per cent among women aged 15-49 years and 45.7 per cent in 2010 to 36.2 per cent among men aged 15-49 years.
Based on this, the NSF 2018-2023 therefore identifies stigma and discrimination as a major hurdle for the attainment of the national vision of ending AIDS by 2022.
The 2011 Stigma
Index Report
As the country seeks to end AIDS by 2022, there is a realisation that the target can only be attained when the pivotal role of PLHIV is recognised and encouraged.
With the NSF 2018-2023 recognising the need to eliminate HIV stigma and discrimination as a key pillar to Ending AIDS by 2022, the NSF 2018-2023 includes a programme for HIV related stigma and discrimination and human rights, with a target to reduce stigma to less than 10 per cent by 2023.
The first Stigma Index Report was pioneered in 2011by the Swaziland National Network of People Living with HIV and AIDS (SWANNEPHA).
It assessed the prevalence and type of stigma and discrimination in the country by collecting experiences of PLHIV in communities in relation to stigma, discrimination at home, at work, in relationships and even measured the extent of self or personal stigma.
Specifically, the stigma index determined and documented the experiences of stigma among PLHIV in relation to health care, employment, sexual and reproductive health rights and measured the (negative) impact of stigma on interventions implemented in the country.
Some of the key findings of the Stigma Index Report include the following:
n In relationships, eight per cent of the respondents indicated that they had been subjected to psychological pressure or manipulation by their spouses or partners, wherein their HIV status was used against them. 20 per cent of the respondents indicated experiencing situations where their spouse or partner, members of their household was discriminated because of the respondent’s positive HIV status;
n About 5.5 per cent of the respondents stated that they had experienced discrimination by other PLHIV;
n There were 2.8 per cent respondents who alluded to having the experience of being refused employment or a work opportunity as a result of their HIV positive status.
n At least 2.3 per cent of the respondents reported having their job description or nature of their work changed or refused promotion as a result of their HIV status;
n There were 4.6 per cent who were denied dental care because of their HIV status; 1.1 per cent were denied family planning services; and 3.7 per cent were denied sexual reproductive health services.
Recent Stigma Index Report preliminary report
The NSF 2018-2023 identifies the need to eliminate HIV stigma and discrimination as a key pillar to Ending AIDS by 2022 and includes a programme for HIV related stigma and discrimination and human rights, with a target to reduce stigma to less than 10 per cent by 2023.
Consequently, the HIV responserecently engaged in a critical assessment of HIV related stigma, discrimination and human rights among PLHIV, using The People Living with HIV Stigma Index Guideline.
The purpose of the assessment was to measure where and when stigma and discrimination against people living with HIV and AIDS occurs; to measure stigma and discrimination and its impact on the response to HIV especially disclosure and treatment; to identify promising approaches to stigma and discrimination that can be taken to scale to achieve sufficient impact across the country, to generate evidence and identify gaps in HIV programs that may fuel stigma and discrimination; to assess and document the experiences of PLHIV in general and key populations living with HIV, regarding stigma and discrimination and profile PLHIV on matters related to human rights.
The preliminary findings show that:
n Of the respondents asked about any experiences related to stigma and discrimination from health care workers in the past 12 months. Only less than 10 per cent of respondents reported experiencing stigma and discrimination from health care workers.
n Of those asked if they believed their medical records were kept confidential when they go to seek health care services, most respondents, about 79 per cent reported that they have trust that their medical records were kept confidential.
n Among those who self-identified themselves as sex workers, 55 per cent indicated that they had not experienced stigma and discrimination because of sex work.
n About 38 per cent indicated that they had been verbally harassed.
n 52 per cent of sex workers indicated that family and friends did not know that they were sex workers.
n About 88 per cent of sex workers were on HIV treatment.
Though there is a notable reduction in stigma and discrimination, the preliminary results point out that disclosure is still a problem.
This undermines preventative strategies, affects health seeking behaviour, and drives the epidemic underground, which perpetuates the vicious and silent nature of the epidemic.
share story
Post Your Comments Below
On Saturday One Billion Rising Eswatini held a mountain circle hike in partnership with the Proje...

Nurses and other members of the medical staff at the Raleigh Fitkin Memorial (RFM) Hospital have ...
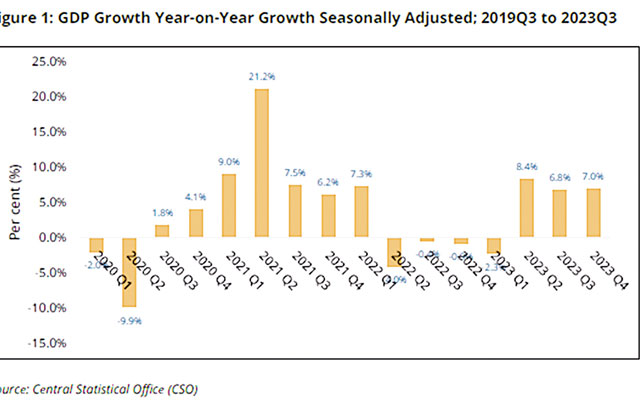
Eswatini's economic activity, measured by Gross Domestic Product (GDP), grew at a steady pace of ...

There is tension mounting between members of Parliament and their constituency headmen, who are n...
All material © Swazi Observer. Material may not be published or reproduced in any form without prior written permission.
Design by Real Image Internet